New York No Fault Doctors
Serving Brooklyn, Bronx, Manhattan, Queens, Staten Island, and Long IslandIf you have been involved in a motor vehicle accident, and in need of medical care, then look no further.

New York No Fault Doctors – Parkchester
Denny Rodriguez, MD
1855 Westchester Ave Bronx, NY 10472
(347) 960-5301

Comprehensive Post-Accident Medical Care in Parkchester, Bronx
Board-Certified Multi-Specialty Practice | Evidence-Based Treatment Protocols | Experienced in New York No-Fault System
About Our Parkchester Practice
New York No Fault Doctors – Parkchester is a comprehensive multi-specialty medical practice dedicated to treating injuries sustained in motor vehicle accidents and workplace incidents. Located at 1855 Westchester Avenue in the heart of Parkchester, our practice combines board-certified medical expertise with a thorough understanding of New York’s no-fault insurance system to provide seamless, patient-centered care.
Under the medical direction of Dr. Dennis Rodriguez, MD, our practice brings together specialists in physical medicine and rehabilitation, orthopedics, neurology, pain management, and therapeutic services to address the complex nature of accident-related injuries. We recognize that motor vehicle accidents can result in multiple injury types affecting different body systems, and our integrated approach ensures you receive coordinated, comprehensive care under one roof.
Meet Dr. Dennis Rodriguez, MD
Dr. Dennis Rodriguez serves as the medical director of our Parkchester location. Dr. Rodriguez brings extensive experience in treating post-traumatic injuries and coordinating complex care plans for accident victims. His patient-centered philosophy emphasizes thorough diagnostic evaluation, evidence-based treatment protocols, and clear communication throughout the recovery process.
Medical Credentials & Expertise:
- Board-certified physician with specialized training in accident and injury medicine
- Extensive experience treating motor vehicle accident injuries across all severity levels
- Expert in musculoskeletal rehabilitation and post-traumatic recovery
- Comprehensive knowledge of New York State no-fault insurance medical requirements
- Collaborative approach working with our full team of specialists to develop integrated treatment plans
Dr. Rodriguez understands that accident injuries often involve multiple affected areas—a rear-end collision might cause both cervical spine injury and shoulder trauma, for example. His diagnostic approach looks at the complete picture of your injuries to develop treatment strategies that address all affected systems, not just individual symptoms.
Understanding Motor Vehicle Accident Injuries: An Evidence-Based Approach
Motor vehicle accidents create unique injury patterns due to the sudden forces involved. Understanding the mechanism of your injury is the first step toward effective treatment and recovery.
Common Injury Types We Treat
Cervical Spine Injuries (Whiplash-Associated Disorders)
Cervical acceleration-deceleration injuries, commonly called whiplash, occur when the head rapidly moves forward and backward during an impact. This motion can damage soft tissues, intervertebral discs, facet joints, and nerve structures in the neck.
Injury Mechanism: During rear-end collisions, the torso is pushed forward by the seat while the head initially lags behind, creating hyperextension. The head then snaps forward into hyperflexion. This sequence happens in milliseconds but can strain ligaments, tear muscle fibers, and stress spinal joints beyond their normal range of motion.
Symptoms & Diagnosis: Patients may experience neck pain and stiffness, headaches (especially at the base of the skull), shoulder pain, dizziness, and difficulty concentrating. Symptoms don’t always appear immediately—many patients feel relatively normal for 12-48 hours before pain and stiffness develop as inflammation increases. Our diagnostic approach includes detailed physical examination, range of motion testing, neurological assessment, and imaging when indicated (X-rays to rule out fractures, MRI for soft tissue evaluation).
Treatment Protocol: Evidence-based treatment begins with pain management and early mobilization. Contrary to older approaches, prolonged immobilization in a cervical collar can delay recovery. Our protocol typically includes:
- Initial phase (weeks 1-2): Pain control through appropriate medications, ice/heat therapy, gentle range-of-motion exercises
- Active recovery phase (weeks 3-8): Progressive physical therapy focusing on strengthening cervical and upper back muscles, postural correction, gradual return to normal activities
- Maintenance phase (ongoing): Home exercise programs, ergonomic modifications, periodic reassessment
Most whiplash injuries improve significantly within 6-12 weeks with appropriate treatment, though some patients experience longer recovery periods depending on injury severity and individual factors.
Lumbar Spine Injuries
Lower back injuries are extremely common in motor vehicle accidents, particularly in side-impact and rear-end collisions. The lumbar spine bears significant force during accidents and is vulnerable to multiple injury types.
Injury Types:
- Muscular strains: Overstretching or tearing of the muscles and tendons supporting the lower back
- Ligamentous sprains: Damage to ligaments connecting vertebrae
- Disc injuries: Herniation or bulging of intervertebral discs, which can compress spinal nerves
- Facet joint injuries: Damage to the small joints between vertebrae that guide spinal movement
Diagnostic Approach: We conduct thorough evaluation including pain pattern assessment, neurological examination for nerve involvement, straight leg raise testing, and imaging studies when clinically indicated. MRI provides the most detailed view of soft tissue structures, while CT scans better visualize bone.
Treatment Strategy: Our approach adapts to injury severity:
- Acute muscular injuries: Anti-inflammatory medications, muscle relaxants when needed, ice therapy initially followed by heat, gentle stretching and early mobilization
- Disc herniations: Physical therapy focusing on core stabilization, directional preference exercises (McKenzie method), epidural steroid injections for significant nerve compression when conservative care proves insufficient
- Chronic pain management: Multimodal approach including physical therapy, therapeutic exercises, potential trigger point injections, patient education on biomechanics and injury prevention
Traumatic Brain Injuries & Concussions
Even “minor” accidents can result in concussion—a form of mild traumatic brain injury caused by rapid acceleration or deceleration forces to the brain. Concussions don’t always involve loss of consciousness; in fact, most don’t.
Recognition & Symptoms: Our neurological specialists assess for concussion symptoms including headache, dizziness, balance problems, nausea, sensitivity to light or noise, difficulty concentrating, memory problems, irritability, sleep disturbances, and feeling mentally “foggy.”
Diagnostic Protocol: Concussion diagnosis relies primarily on clinical evaluation rather than imaging (CT and MRI are typically normal in concussion). Our neurologists conduct detailed cognitive testing, balance assessment, and symptom tracking using standardized concussion assessment tools.
Recovery Approach: Current evidence supports graduated return to activities:
- Cognitive and physical rest (48-72 hours)
- Light activity below symptom threshold
- Moderate activity as tolerated
- Heavy non-contact activity
- Full contact practice (for athletes)
- Return to normal activities
Progression only occurs when the patient can complete each stage without symptom exacerbation. Most concussion patients recover within 7-14 days, though some experience post-concussive syndrome requiring longer management.
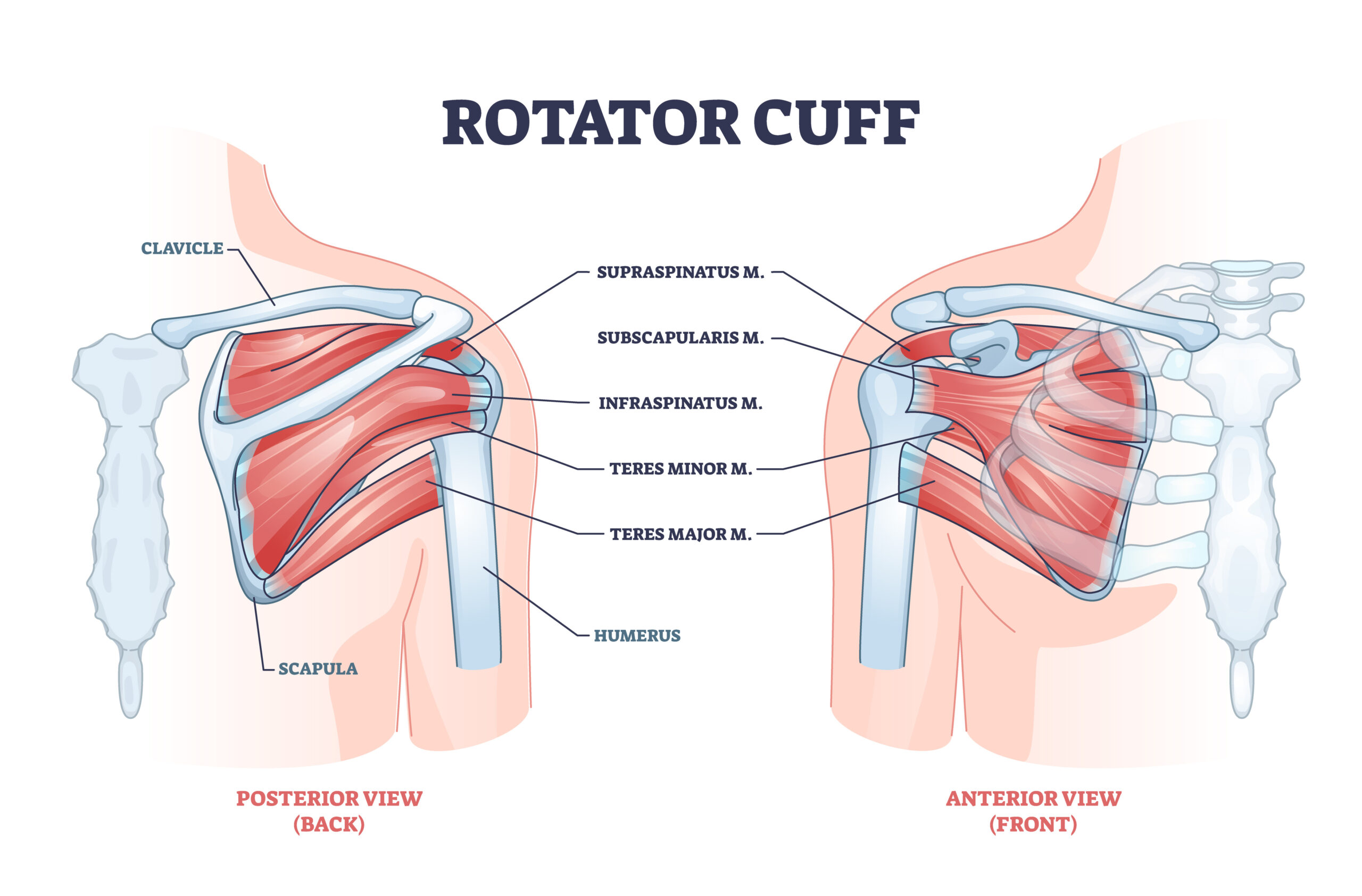
Shoulder Injuries
The shoulder complex frequently sustains injury in motor vehicle accidents, particularly from seatbelt forces, impact with interior vehicle surfaces, or the forceful bracing motion drivers make against the steering wheel.
Common Shoulder Injuries:
- Rotator cuff strains or tears: The four muscles stabilizing the shoulder can be stretched or torn
- Labral injuries: Damage to the cartilage rim surrounding the shoulder socket
- Acromioclavicular (AC) joint sprains: Injury to the joint connecting the collarbone to the shoulder blade
- Biceps tendon injuries: Inflammation or tears of the biceps tendon
Examination & Diagnosis: Our orthopedic specialists conduct detailed shoulder examination including range of motion testing, strength assessment, specific impingement tests, and stability testing. MRI arthrography provides detailed visualization when surgical intervention may be considered.
Treatment Pathways: Many shoulder injuries respond well to conservative treatment including physical therapy focused on rotator cuff strengthening, scapular stabilization, and range of motion restoration. Severe tears or persistent instability may require orthopedic surgical consultation, which we coordinate when needed.
Soft Tissue Injuries
Soft tissue injuries—sprains, strains, and contusions affecting muscles, tendons, and ligaments throughout the body—are nearly universal in motor vehicle accidents. While sometimes dismissed as “minor,” these injuries can cause significant pain and functional limitation.
Understanding Soft Tissue Healing: Soft tissue healing occurs in three overlapping phases:
- Inflammatory phase (0-5 days): Pain, swelling, heat as the body initiates the healing response
- Proliferative phase (5 days-3 weeks): New collagen fibers form to repair damaged tissue
- Remodeling phase (3 weeks-12 months): Tissue strengthens and organizes along lines of stress
Treatment Aligned with Healing Phases:
- Inflammatory phase: RICE protocol (rest, ice, compression, elevation), pain control, gentle range of motion to prevent stiffness
- Proliferative phase: Progressive loading, strengthening exercises, manual therapy
- Remodeling phase: Functional training, sport or activity-specific rehabilitation, prevention strategies
Understanding these phases helps patients maintain realistic expectations and participate actively in their recovery.
Our Multi-Specialty Treatment Approach
Effective accident injury treatment requires coordinated care across multiple specialties. Our practice integrates the following services to provide comprehensive treatment plans tailored to each patient’s injury pattern.
Physical Medicine & Rehabilitation (Physiatry)
Our physiatrists serve as the cornerstone of care coordination for complex injury cases. These specialists focus on restoring function and quality of life through non-surgical approaches. Physiatrists excel at diagnosing the full extent of musculoskeletal and neurological injuries, then developing integrated treatment plans that may involve multiple therapeutic modalities.
When Physiatry Is Indicated: Patients with multi-system injuries, chronic pain developing after acute injury, functional limitations affecting daily activities, or those requiring coordination among multiple treatment providers benefit most from physiatric care.
Orthopedic Care
Our orthopedic specialists diagnose and treat injuries to bones, joints, muscles, tendons, and ligaments. While orthopedists can perform surgery when necessary, many accident injuries respond well to conservative orthopedic management.
Orthopedic Services:
- Fracture evaluation and management
- Joint injury assessment and treatment
- Diagnostic injections for pain relief and diagnostic clarification
- Coordination with physical therapy for optimal recovery
- Surgical consultation and referral when conservative care proves insufficient
Neurology
Neurological evaluation is crucial for patients experiencing headaches, dizziness, numbness, tingling, cognitive changes, or other symptoms suggesting nervous system involvement. Our neurologists specialize in diagnosing and managing both central nervous system injuries (brain and spinal cord) and peripheral nerve injuries.
Neurological Assessment Tools:
- Comprehensive neurological examination
- Electrodiagnostic testing (EMG/NCV) for nerve injury evaluation
- Cognitive assessment for concussion or mild traumatic brain injury
- Coordination with imaging specialists for MRI/CT interpretation
- Medication management for neuropathic pain and headache
Pain Management
Chronic pain developing after accidents requires specialized expertise. Our pain management specialists use multimodal approaches to address both acute post-accident pain and persistent pain conditions.
Pain Management Techniques:
- Medication optimization balancing pain relief with safety and minimal side effects
- Interventional procedures including trigger point injections, joint injections, and nerve blocks when indicated
- Coordination with physical therapy and rehabilitation services
- Patient education on pain science and self-management strategies
- Minimally invasive procedures for targeted pain relief
Physical Therapy
Physical therapy forms the foundation of functional recovery for most accident injuries. Our licensed physical therapists develop individualized programs based on injury type, severity, and patient goals.
Physical Therapy Services:
- Initial evaluation and functional assessment
- Manual therapy techniques to restore mobility
- Therapeutic exercises for strength, flexibility, and endurance
- Modalities including heat, ice, ultrasound, and electrical stimulation when appropriate
- Functional training for return to work, sports, or daily activities
- Home exercise program development and progression
- Ergonomic and body mechanics education
Evidence strongly supports active physical therapy over passive treatments alone. Our therapists emphasize patient education and active participation in recovery.
Chiropractic Care
Chiropractic treatment focuses on spinal alignment and joint function. Our chiropractors use manual adjustments and mobilization techniques to address joint restrictions, improve spinal mechanics, and reduce pain.
Chiropractic Approaches:
- Spinal manipulation to restore joint mobility
- Soft tissue therapy for muscle tension and trigger points
- Therapeutic exercises and stretching
- Postural assessment and correction
- Collaborative care with other specialists as needed
Research supports chiropractic care for certain spine conditions, particularly mechanical neck and low back pain. We ensure all treatment recommendations are evidence-based and appropriate for your specific condition.
Acupuncture
Acupuncture offers an alternative therapeutic approach for pain management and healing support. This traditional Chinese medicine technique involves inserting thin needles at specific points to promote healing and pain relief.
Acupuncture Applications:
- Pain reduction for various injury types
- Inflammation management
- Muscle tension relief
- Headache treatment
- Stress and anxiety reduction during recovery
Current research suggests acupuncture may stimulate endorphin release, modulate pain signals, and promote local blood flow to injured areas. Many patients find acupuncture a valuable complement to conventional treatment.

Understanding New York’s No-Fault Insurance System
New York operates under a no-fault auto insurance system designed to ensure accident victims receive prompt medical care regardless of who caused the accident. Understanding this system helps you access appropriate treatment without delay.
How No-Fault Insurance Works
Under New York law, your own auto insurance policy provides coverage for medical treatment, lost wages, and other expenses resulting from accident injuries, regardless of fault. This system eliminates the need to prove fault before receiving treatment and ensures faster access to care.
Coverage Basics:
- Minimum coverage: $50,000 per person (higher limits available)
- Covers necessary medical treatment, rehabilitation, and certain other expenses
- No deductibles or copayments for covered medical services
- Coverage extends to passengers, pedestrians, and cyclists injured by motor vehicles
Filing Requirements & Timelines
New York’s no-fault system includes strict filing deadlines:
30-Day Application Deadline: You must file a no-fault application (Form NF-2) within 30 days of the accident. Failure to meet this deadline may result in denial of coverage.
Treatment Documentation: All medical providers must submit proper documentation including initial examination forms (NF-3) and billing statements (NF-4) within prescribed timeframes.
Ongoing Treatment: Additional claims for continued treatment must be submitted promptly with appropriate medical necessity documentation.
Our Role in the Insurance Process
We handle all aspects of no-fault insurance documentation and billing, allowing you to focus on recovery rather than paperwork. Our experienced administrative team:
- Completes all required no-fault forms accurately and on time
- Submits claims directly to insurance carriers
- Responds to insurance company requests for additional information
- Documents medical necessity for all recommended treatments
- Communicates with adjusters regarding treatment plans and coverage questions
- Ensures you’re not billed for covered services
This expertise ensures your legitimate medical expenses are covered without out-of-pocket costs for covered treatments.
Workers’ Compensation Coverage
For work-related accidents or injuries sustained while performing job duties, workers’ compensation insurance provides coverage separate from no-fault auto insurance. Our practice accepts workers’ compensation insurance and manages all associated documentation and billing requirements.
Workers’ Compensation Services:
- Initial injury evaluation and documentation
- Treatment coordination with employers and insurance carriers
- C-4 and other required form completion
- Independent medical examination (IME) preparation and support
- Return-to-work assessments and modified duty recommendations
- Ongoing treatment within workers’ compensation guidelines
Serving the Parkchester Community
Parkchester is one of the Bronx’s most distinctive neighborhoods, known for its planned community design, diverse population, and strong sense of community. Our practice is proud to serve Parkchester residents and the surrounding areas.
About Parkchester
Parkchester was developed in the late 1930s and early 1940s as one of the first planned communities in New York City. The neighborhood features a distinctive architectural style with multiple apartment complexes arranged around central courtyards and green spaces. Today, Parkchester is home to a vibrant, diverse community with excellent access to public transportation, shopping, and services.
Parkchester Demographics & Character:
- Population: Approximately 35,000 residents
- Diversity: One of the Bronx’s most diverse neighborhoods with significant Hispanic, African American, and Asian populations
- Transportation: Excellent subway access via 6 train (Parkchester station)
- Major Corridors: Westchester Avenue, White Plains Road, Metropolitan Avenue
- Notable Features: Parkchester apartment complex, Hugh J. Grant Circle, Bronx River Greenway access
Neighborhoods We Serve
Our Parkchester location is strategically positioned to serve patients throughout the East and Central Bronx. We regularly treat patients from:
East Bronx:
- Parkchester (10462, 10472)
- Westchester Square (10461, 10472)
- Van Nest (10462)
- Morris Park (10461, 10462)
- Pelham Parkway (10461, 10462)
- Throggs Neck (10465)
- Castle Hill (10472, 10473)
- Soundview (10472, 10473)
Central Bronx:
- East Tremont (10460)
- West Farms (10460)
- Belmont (10458, 10457)
- Fordham (10458, 10468)
- Bronx Park (10462)
Other Bronx Areas:
- Allerton (10467)
- Pelham Gardens (10461, 10469)
- Williamsbridge (10467)
- Unionport (10462)
- Schuylerville (10465)
Zip Codes Served
Primary Service Area Zip Codes:
- 10472 (Parkchester, Soundview)
- 10462 (Parkchester South, Van Nest, Morris Park)
- 10461 (Westchester Square, Morris Park East, Pelham Parkway)
- 10473 (Soundview, Castle Hill)
- 10465 (Throggs Neck, Country Club)
- 10460 (West Farms, East Tremont)
- 10472 (Soundview, Clason Point)
Extended Service Area:
- 10458 (Fordham, Belmont)
- 10467 (Allerton, Williamsbridge)
- 10468 (Fordham North, University Heights)
- 10469 (Baychester, Pelham Gardens)
- 10470 (Wakefield, Woodlawn)
Transportation & Accessibility
Our Westchester Avenue location offers convenient access via multiple transportation options:
By Subway:
- 6 train to Parkchester station (3-minute walk to our office)
- Accessible station with elevator service
By Bus:
- Bx4, Bx4A, Bx21, Bx36 buses along Westchester Avenue
- Bx39 along White Plains Road
- Multiple bus routes provide connections from throughout the Bronx
By Car:
- Convenient to Bruckner Expressway (I-278) and Cross Bronx Expressway (I-95)
- Street parking available on surrounding streets
- Municipal parking facilities within walking distance
Accessibility:
- Ground-level entrance with wheelchair access
- Accessible examination rooms and facilities
- Accommodation available for patients with mobility limitations
Common Traffic Accident Patterns in Parkchester
Understanding local traffic patterns helps us anticipate and effectively treat common injury types seen in our patient population.
High-Traffic Corridors & Accident Hotspots
Westchester Avenue: This major east-west corridor carries heavy traffic between the Bronx and Westchester County. Common accident types include:
- Rear-end collisions during rush hour congestion
- Side-impact collisions at busy intersections (White Plains Road, Hugh J. Grant Circle)
- Pedestrian accidents due to high foot traffic near shopping areas
Cross Bronx Expressway (I-95): Though not directly in Parkchester, this heavily congested highway serves as a major route for our patient population. Accidents on the Cross Bronx frequently result in:
- High-speed rear-end collisions
- Multi-vehicle accidents during traffic backups
- More severe injuries due to highway speeds
Bruckner Expressway (I-278): Connecting to the Throgs Neck and Whitestone Bridges, the Bruckner sees significant accident volume:
- Merge-related side-swipe collisions
- Speed-related rear-end impacts
- Commercial vehicle accidents (delivery trucks, work vehicles)
White Plains Road: Heavy commercial and residential traffic creates accident risks:
- Double-parked vehicles causing traffic disruptions and accidents
- Delivery vehicle accidents
- Pedestrian accidents near bus stops and crosswalks
Seasonal & Weather Considerations
The Bronx experiences all four seasons with associated weather challenges that increase accident risk:
Winter Conditions (December-March):
- Ice and snow reduce traction and increase stopping distances
- Black ice on bridges and overpasses
- Reduced visibility during snowfall
- Salt and sand create slippery conditions as snow melts
Summer Heat (June-September):
- Tire blowouts from hot pavement
- Driver fatigue and reduced attention
- Increased motorcycle and bicycle traffic
- Summer thunderstorms creating sudden hazardous conditions
Our providers recognize how accident mechanisms change with seasons and weather, informing our diagnostic approach and treatment planning.
What to Do After a Motor Vehicle Accident
Taking appropriate steps immediately after an accident protects both your health and your insurance coverage rights.
Immediate Steps at the Accident Scene
- Ensure Safety: Move to a safe location if possible; call 911 if anyone is injured
- Call Police: New York law requires police reports for accidents involving injury, death, or property damage exceeding $1,000
- Exchange Information: Collect driver information, insurance details, and contact information from all parties
- Document the Scene: Photograph vehicle damage, road conditions, and accident location if able
- Note Symptoms: Pay attention to how you feel, even if you don’t feel injured immediately
Seeking Medical Care
Seek Medical Evaluation Promptly—Even If You Feel Fine: Many accident injuries don’t produce immediate symptoms. Adrenaline and endorphins released during stressful events can mask pain. Delayed evaluation may complicate both your recovery and insurance claim.
Why Early Evaluation Matters:
- Some injuries worsen without early intervention
- Insurance companies may question delayed treatment
- Early documentation establishes the connection between accident and injury
- Treatment begun early generally results in better outcomes
What to Expect at Your First Visit:
- Comprehensive injury assessment
- Discussion of accident mechanism and symptoms
- Physical examination focused on affected areas
- Diagnostic imaging if clinically indicated
- Development of initial treatment plan
- Completion of required insurance documentation
Insurance Filing & Documentation
Our administrative team guides you through insurance requirements, but understanding the basics helps ensure smooth processing:
Required Documents:
- Police report (obtain from responding officer or precinct)
- Insurance information (your policy and other party’s if available)
- Driver’s license and vehicle registration
- Form MV-104 (Report of Motor Vehicle Accident) if police didn’t respond
No-Fault Claim Filing:
- Complete Form NF-2 (Application for No-Fault Benefits) within 30 days
- Submit to your insurance carrier
- Our office will complete provider forms (NF-3 for initial treatment)
Our Documentation Support:
- We complete all medical provider forms
- Submit claims directly to insurance carriers
- Maintain detailed treatment records
- Respond to insurance requests for information
- Ensure all medical necessity documentation is thorough and timely
Frequently Asked Questions
Q: Do I need to pay out of pocket for treatment?
A: For covered no-fault insurance services, there should be no out-of-pocket costs. New York’s no-fault system requires your auto insurance to pay for medically necessary treatment regardless of fault. We bill insurance directly and handle all documentation.
Q: What if the accident wasn’t my fault?
A: Under New York’s no-fault system, your own insurance covers your medical treatment regardless of who caused the accident. This ensures you receive prompt care without waiting for fault determination. Later, insurance companies may pursue reimbursement from at-fault parties, but this doesn’t affect your access to treatment.
Q: How long do I have to file a no-fault claim?
A: You must file Form NF-2 (Application for No-Fault Benefits) within 30 days of the accident. This deadline is strict—late filing can result in denial of coverage. We help ensure all paperwork is submitted promptly.
Q: What if my symptoms didn’t appear until days after the accident?
A: This is very common. Many accident injuries produce delayed symptoms as inflammation develops and adrenaline wears off. Seek medical evaluation even if symptoms appear days later. Our providers understand delayed-onset injuries and document the connection between accident and symptoms.
Q: Do I need a referral from my primary care doctor?
A: No. Under New York’s no-fault system, you can seek treatment from qualified providers directly without a referral. However, we recommend informing your primary care physician about the accident and your treatment.
Q: How long will my recovery take?
A: Recovery timelines vary based on injury type, severity, and individual factors. Minor soft tissue injuries may improve within 4-8 weeks, while more significant injuries may require several months of treatment. We provide realistic timeframes based on your specific injuries and monitor progress throughout treatment.
Q: What if I need to miss work for treatment?
A: New York’s no-fault insurance covers lost wages under certain circumstances. We provide documentation of medical necessity for your absence when needed. For work-related accidents, workers’ compensation covers both treatment and wage replacement.
Q: Can I choose my own doctors for treatment?
A: Yes. New York allows you to select your medical providers. Many patients choose our practice because of our multi-specialty expertise and experience with the no-fault insurance system.
Q: What if my insurance denies my claim?
A: Insurance denials can occur for various reasons including late filing, lack of medical necessity documentation, or administrative errors. We work with patients to appeal inappropriate denials and ensure documentation supports medical necessity for all recommended treatment.
Q: Will you coordinate with my attorney if I have one?
A: Yes. We regularly work with personal injury attorneys and provide necessary medical documentation, records, and narrative reports when requested. We understand the intersection of medical treatment and legal representation in accident cases.
Schedule Your Appointment Today
If you’ve been injured in a motor vehicle accident or workplace incident, don’t delay seeking appropriate medical care. Our team of specialists at New York No Fault Doctors – Parkchester is ready to provide comprehensive evaluation and evidence-based treatment.
Contact Information:
New York No Fault Doctors – Parkchester 1855 Westchester Avenue Bronx, NY 10472
Phone: (347) 960-5301 Main Line: (888) 511-0625
Office Hours: Tuesday – Thursday: 11:00 AM – 7:00 PM Saturday: Closed Sunday: Closed Evening and weekend appointments available.
What to Bring to Your First Appointment:
- Driver’s license or photo ID
- Auto insurance card
- Police report (if available)
- Any medical records from emergency room or other providers
- List of current medications
- Completed patient forms (available on our website or at check-in)
Our commitment is to provide expert medical care while handling the administrative complexities of New York’s no-fault insurance system, allowing you to focus on what matters most—your recovery. Whether you’re experiencing neck pain after a rear-end collision, back pain from a side-impact crash, or any other accident-related injury, our multi-specialty team has the expertise to help you heal.
Don’t let pain and injury disrupt your life. Call us today at (347) 960-5301 to schedule your comprehensive evaluation with our experienced team.